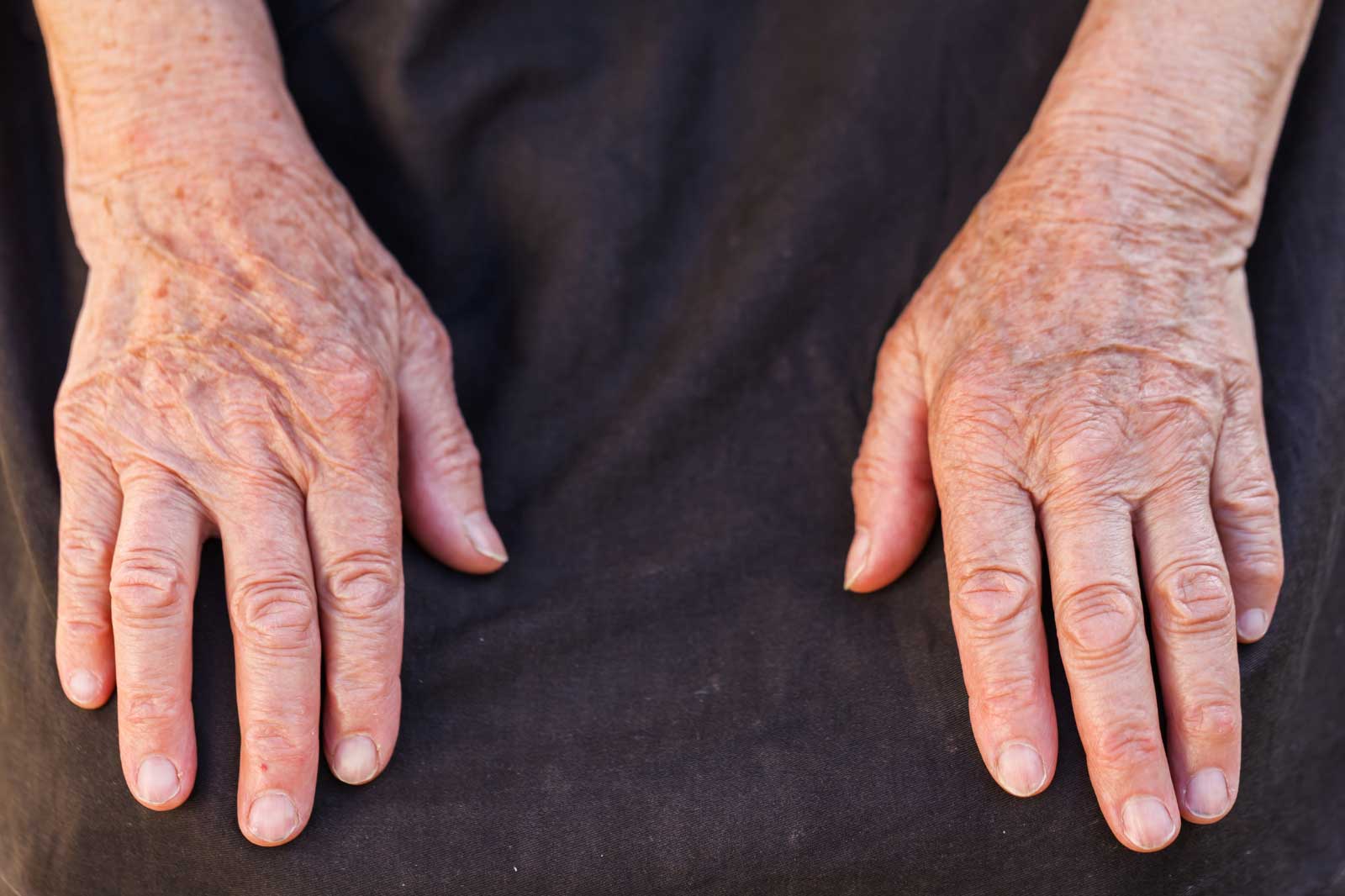
What Is Psoriatic Arthritis? Symptoms, Treatments, and Clinical Trial Options in Tampa Bay
Written by John D. Carter, MD — Board-Certified Rheumatologist and Principal Investigator, Clinical Research of West Florida
Psoriatic arthritis (PsA) is often an underdiagnosed autoimmune condition in the United States. Millions of people live with joint pain, skin flares, and fatigue — often for years — before receiving a correct diagnosis. For those who have it, understanding psoriatic arthritis treatment options, including access to clinical trials evaluating investigational treatments that may help improve disease management for some patients.
At Clinical Research of West Florida (CRWF), we study psoriatic arthritis through clinical research to help advance treatment options. This guide is designed to help patients, caregivers, and families in Tampa Bay and the greater Pinellas County area understand PsA more fully — and explore whether a clinical trial could be the right next step.
What Is Psoriatic Arthritis (PsA)?
Psoriatic arthritis is a chronic autoimmune disease that causes inflammation in the joints and, in most cases, occurs alongside psoriasis — a skin condition that produces red, scaly, itchy patches. PsA develops when the immune system mistakenly attacks healthy joint tissue, triggering pain, swelling, and stiffness that can become progressively disabling without proper treatment.
Unlike osteoarthritis, which is a mechanical “wear and tear” condition managed by orthopedic physicians, PsA is an inflammatory disease typically treated by a rheumatologist or dermatologist. It is part of a broader family of conditions known as spondyloarthropathies, which share features like enthesitis (inflammation where tendons meet bone) and axial involvement of the spine.
Approximately 30% of people with psoriasis will develop psoriatic arthritis at some point in their lives, though PsA can also occur in individuals with minimal or no visible skin disease.
What Are the Symptoms of Psoriatic Arthritis?
PsA presents differently from person to person, which is part of what makes it difficult to diagnose. The most common symptoms include:
Joint Symptoms
- Swollen, painful, warm joints — often asymmetrical
- Stiffness, especially in the morning or after periods of inactivity
- Swollen fingers or toes that take on a “sausage-like” appearance (dactylitis)
- Lower back pain or stiffness from spinal involvement (spondylitis)
- Reduced range of motion over time if untreated
Skin and Nail Symptoms
- Red, scaly plaques on the skin (psoriasis)
- Nail pitting, ridging, or separation from the nail bed (onycholysis)
Systemic Symptoms
- Fatigue and generalized malaise
- Eye inflammation (uveitis) in some patients
- Tenderness where tendons or ligaments attach to bone (enthesitis)
Because these symptoms can overlap with rheumatoid arthritis, gout, and reactive arthritis, an accurate diagnosis requires evaluation by a rheumatologist, often supported by blood tests, imaging, and a thorough skin and joint examination.
How Is Psoriatic Arthritis Diagnosed?
There is no single definitive test for PsA. Diagnosis is largely clinical — meaning it relies on the physician’s assessment of your full symptom picture, history, and test results. At CRWF, our diagnostic approach typically includes:
- A thorough medical history and physical examination of affected joints and skin
- Laboratory tests including inflammatory markers (CRP, ESR) and rheumatoid factor — which is often negative in PsA, distinguishing it from RA
- Imaging studies such as X-rays, ultrasound, or MRI to detect joint damage and inflammation
- A dermatologic review to assess the extent of psoriatic skin involvement
Early diagnosis matters enormously. Untreated PsA can lead to irreversible joint destruction and significantly impaired quality of life.
What Are the Current Treatment Options for Psoriatic Arthritis?
PsA treatment has evolved dramatically over the past two decades, moving from symptom management to genuine disease modification. The goal today is not just to relieve pain — it is to halt joint damage, achieve remission, and preserve long-term function.
Non-steroidal anti-inflammatory drugs (NSAIDs) are often a first step for mild symptoms. They reduce inflammation and pain but do not prevent joint damage and are not suitable for all patients, particularly those with cardiovascular or gastrointestinal concerns.
Conventional DMARDs (Disease-Modifying Anti-Rheumatic Drugs) such as methotrexate, sulfasalazine, and leflunomide are used for moderate disease. They slow progression by suppressing immune activity, though their effect on skin disease can be variable.
Biologic therapies have transformed outcomes for moderate-to-severe PsA. These targeted agents include:
- TNF inhibitors (adalimumab, etanercept, certolizumab)
- IL-17 inhibitors (secukinumab, ixekizumab)
- IL-12/23 inhibitors (ustekinumab)
- IL-23 inhibitors (guselkumab, risankizumab)
Biologics directly target the cytokines driving inflammation, often producing dramatic improvements in both joint and skin symptoms.
JAK inhibitors (tofacitinib, upadacitinib) represent an oral targeted therapy option for patients who have not responded adequately to biologics. They inhibit the Janus kinase signaling pathway inside immune cells, offering a convenient alternative to injectable biologics.
Despite these advances, many patients with PsA do not achieve full remission on available therapies. This is precisely why clinical trial research remains essential — and why CRWF is actively investigating next-generation treatments.
What New Treatments Are Being Investigated for Psoriatic Arthritis?
The pipeline for PsA research is one of the most active in rheumatology. Investigators are pursuing several promising avenues:
Researchers are exploring dual-pathway inhibitors that simultaneously block multiple inflammatory cytokines, potentially offering broader disease control than current single-target biologics. Early clinical data on agents targeting both IL-17 and IL-23 pathways have shown promising outcomes in patients with refractory psoriatic disease.
Selective tyrosine kinase inhibitors, specifically targeting TYK2 (tyrosine kinase 2), are emerging as a new oral class. Deucravacitinib, already FDA-approved for psoriasis, is being studied in PsA, offering a potentially safer side-effect profile than older JAK inhibitors.
Precision medicine approaches using biomarkers to predict individual treatment response are also gaining traction. Identifying which patients are most likely to respond to specific biologics — before committing to a treatment — could eliminate the months-long trial-and-error process that burdens many PsA patients today.
How Do Clinical Trials for Psoriatic Arthritis Work?
At CRWF, our psoriatic arthritis clinical trials are structured, regulated research studies designed to evaluate the safety and efficacy of emerging therapies. Participation is entirely voluntary, and patients may withdraw at any time without affecting their standard medical care.
The process begins with an eligibility screening — a brief online form or phone conversation to determine whether you meet the study’s inclusion criteria. If you qualify, you’ll meet with our research team, review and sign an informed consent document, complete baseline health assessments, and begin the study protocol under close clinical supervision.
For our current PsA trials, participation involves up to 20 office visits over 52 weeks. If eligible, all study-related care, lab work, and exams are provided at no cost. Eligible participants may receive compensation up to $2,000 for their time and travel.
CRWF’s current psoriatic arthritis studies are officially registered with the U.S. National Library of Medicine. Full details, including eligibility criteria and study locations, are available at ClinicalTrials.gov under study numbers NCT06865105, NCT07223138, and NCT07286058. View our Psoriatic Arthritis study page to learn more and begin your enrollment.
Who Is Eligible to Join a Psoriatic Arthritis Clinical Trial at CRWF?
General eligibility criteria for our current PsA studies include:
- 18 years of age or older
- Confirmed diagnosis of psoriasis or psoriatic arthritis
- Active psoriatic disease activity
- Currently taking medications for psoriatic disease
CRWF operates conveniently located research facilities in both Clearwater (2147 NE Coachman Road) and Tampa (605 N. Howard Ave.), making participation accessible to patients across the Tampa Bay area.
What Are the Benefits of Joining a Psoriatic Arthritis Trial at CRWF?
There are meaningful reasons why patients with PsA choose to participate in clinical research beyond compensation alone:
- Early access to investigational therapies not yet available to the general public
- Comprehensive health monitoring including physical exams, lab work, and specialist oversight
- All study-related costs covered — no insurance required
- Direct contribution to the advancement of treatments that could benefit future PsA patients worldwide
At CRWF, we bring over 30 years of Tampa Bay clinical trial experience and the direct oversight of board-certified rheumatologists who treat PsA patients in practice every single day. Our participants are not just enrolled in a study — they are partners in research.
Living Well With Psoriatic Arthritis
Medication is only part of the picture. Long-term wellbeing for PsA patients also depends on lifestyle management.
Regular low-impact exercise — including swimming, walking, and cycling — helps maintain joint flexibility and reduce stiffness without aggravating inflamed tissue. An anti-inflammatory diet rich in omega-3 fatty acids, leafy greens, and antioxidants can complement pharmacological treatment by reducing systemic inflammatory load.
Stress management is particularly important in PsA because emotional and physical stress are well-documented triggers for flares. Cognitive behavioral therapy, mindfulness practices, and peer support groups can help patients build resilience and manage the psychological burden of chronic disease.
Physical and occupational therapy play a vital role in preserving joint function, preventing deformity, and adapting daily activities to reduce pain. For patients with significant spinal involvement, targeted core-strengthening programs have been shown to meaningfully reduce axial symptoms.
Frequently Asked Questions About Psoriatic Arthritis
Is psoriatic arthritis the same as rheumatoid arthritis?
No. While both are autoimmune forms of inflammatory arthritis, PsA is linked to psoriasis, is often seronegative (rheumatoid factor negative), and affects the joints in distinct patterns — including the spine, and characteristically the distal finger joints. The treatment landscape overlaps significantly, but the two conditions have important differences in diagnosis, classification, and monitoring.
Can psoriatic arthritis go into remission?
Yes. With appropriate treatment — particularly biologic therapy — many patients achieve low disease activity or full remission. Clinical trials are focused on improving these remission rates and sustaining them over time.
Does psoriasis always come before psoriatic arthritis?
Not always. In most cases, skin psoriasis precedes joint disease by 10 or more years. However, in about 15% of patients, joint symptoms develop before or alongside skin findings, which can complicate and delay diagnosis.
Is it safe to join a clinical trial?
Yes, when conducted at a regulated research facility like CRWF. All trials are overseen by an Institutional Review Board (IRB), monitored for participant safety, and adhere to FDA regulations and Good Clinical Practice guidelines. Participants may receive regular study-related health evaluations, and all adverse events are carefully documented and addressed.
Take the Next Step
If you are living with psoriatic arthritis in the Tampa Bay area and are interested in exploring clinical trial participation, we encourage you to learn more about CRWF’s currently enrolling studies. A brief eligibility form is all it takes to find out if you qualify — and you may be eligible to participate in a study that includes investigational treatment and study-related care.
View CRWF’s Psoriatic Arthritis Clinical Trial →
For questions, contact our Clearwater office at 727-466-0078 or our Tampa office at 813-870-1292.
About the Author: John D. Carter, MD is a board-certified physician in Internal Medicine and Rheumatology with over 20 years of experience in academic medicine and clinical research. He serves as Principal Investigator at Clinical Research of West Florida and has led Phase II–IV clinical trials across autoimmune, inflammatory, and multisystem conditions.
Carter JD, Taurog JD. Psoriatic Arthritis. In Harrison’s Principles of Internal Medicine (19th Edition). McGraw Hill Publishing, Philadelphia, PA. 2017.
Harrison’s Principles of Internal Medicine is the top rated internal medicine textbook in the country.